News & Events
Read about BME’s Latest Activities
-
BME Student Tirth Patel Receives the Barry Goldwater Scholarship
Established in 1986 by the U.S. Congress, the Goldwater Scholarship provides support for highly qualified undergraduates who plan to pursue a PhD and research career in STEM fields. It provides $7,500 for students in support of their junior and/or senior year of study.
-

AMPED Students Present Product Concepts in Culminating Team Project
The presentations were the culmination of the Biomedical Product Realization Practicum course, which is a design-build-test sequence in which student teams work with a clinical mentor to solve a current clinical problem.
-

BME GAAP Team Receives Claudia Joan Alexander Trailblazer Award from WISE
The Claudia Joan Alexander Trailblazer Award is given to an individual or team for the development or implementation of a program, innovation, or intervention (within the last 3 years) that supports equity in STEM at U-M.
-

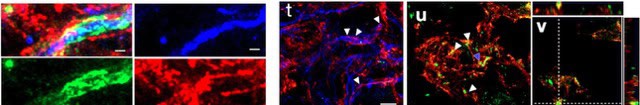
Spatial atlas of the human ovary with cell-level resolution will bolster reproductive research
Most human oocytes never get a chance to mature into eggs — a new study sheds light on why
Recent Posts
-
The BME Exchange Provides Students With Opportunities to Connect with Professionals
-
Maria Coronel Receives JDRF Innovator Award
-
U-M BME’s Rachael Schmedlen Shares Knowledge Abroad as Part of US Africa Teaching Fellows Program
-
Professor Claude M. Steele Highlights ‘Churn’ in His Seminar
-
U-M BME Doctoral Student to Present at Rising Stars Conference on Computational and Data Sciences
-
BME Exchange Provides Networking Opportunities with Alumni Presenters
In the News
CBS News Detroit
February 1
BME’s Cindy Chestek discussed the pros and cons of neural implants with regard to the recent announcement of Elon Musk’s Neuralink trials using the first human implant.
National Association of Advisors for the Health Professions
January 8, 2024
U-M BME’s Rachel Patterson, Student Administration Manager, is featured in the National Association of Advisors for the Health Professions website magazine discussing the advantages an engineering degree can provide for students pursuing health-related careers.
Events
BME SYMPOSIUM WITH GLENN V. EDMONSON LECTURE
KEYNOTE: Dr. Karl Jepsen
MAY 8, 2024, 9:30 a.m.-5:30 p.m.
NCRC BUILDING 18